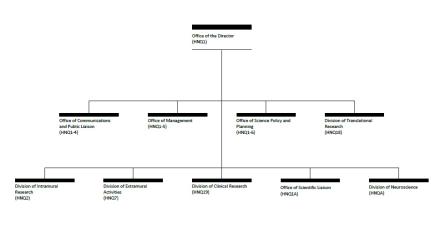
- Organization Chart
- Appropriation Language
- Amounts Available for Obligation
- Budget Graphs
- Authorizing Legislation
- Appropriations History
- Justification of Budget Request
- Detail of Full-Time Equivalent Employment (FTE)
- Detail of Positions
Organization Chart
National Institutes of Health
National Institute of Neurological Disorders and Stroke
For carrying out section 301 and title IV of the PHS Act with respect to neurological disorders and stroke, $1,781,056,000.
Amounts Available for Obligation 1
(Dollars in Thousands)
| Source of Funding | FY 2017 Final |
FY 2018 Annualized CR | FY 2019 President's Budget2 |
|---|---|---|---|
| Appropriation | $1,783,654 | $1,783,654 | $1,838,556 |
| Mandatory Appropriation: (non-add) | |||
| Type 1 Diabetes | (0) | (0) | (0) |
| Other Mandatory financing | 0 | (0) | (0) |
| Rescission | 0 | -12,113 | 0 |
| Sequestration | 0 | 0 | 0 |
| Secretary's Transfer | -3,894 | 0 | 0 |
| Subtotal, adjusted appropriation OAR HIV/AIDS Transfers |
$1,779,760 -1,072 |
$1,771,541 0 |
$1,838,556 0 |
| Subtotal, adjusted budget authority Unobligated balance, start of year Unobligated balance, end of year |
$1,778,688 0 0 |
$1,771,541 0 0 |
$1,838,556 0 0 |
| Subtotal, adjusted budget authority Unobligated balance lapsing |
$1,778,688 -4 |
$1,771,541 0 |
$1,838,556 0 |
| Total obligations | $1,778,684 | $1,771,541 | $1,838,556 |
1 Excludes the following amounts for reimbursable activities carried out by this account:
FY 2017 - $15,631 FY 2018 - $16,241 FY 2019 - $16,636
2 Includes $57.500 million derived bv transfer from the NIH Innovation Account
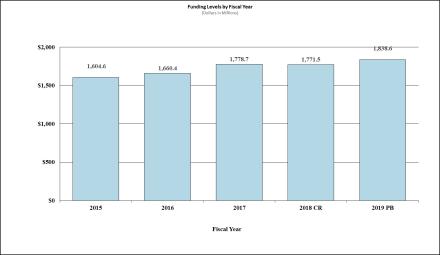
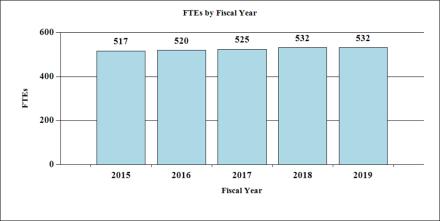
Fiscal Year 2019 Budget Graphs
History of Budget Authority and FTE's:
Authorizing Legislation
| PHS Act/ Other Citation |
U.S. Code Citation |
2018 Amount Authorized |
F Y 2018 Annualized CR |
2019 Amount Authorized |
F Y 2019 PB |
|
|---|---|---|---|---|---|---|
| Research and Investigation | Section 301 | 42§241 | Indefinite | $1,771,541,206 | Indefinite | $1,838,556,000 |
| National Institute of Neurological Disorders and Stroke |
Section 401(a) | 42§281 | Indefinite | Indefinite | ||
| Total, Budget Authority | $1,771,541,206 | $1,838,556,000 |
Appropriations History
| Fiscal Year | Budget Estimate to Congress | House Allowance | Senate Allowance | Appropriation |
|---|---|---|---|---|
| 2009 | $1,545,397,000 | $1,598,521,000 | $1,588,405,000 | $1,593,344,000 |
| Rescission | $0 | |||
| Supplemental | $8,212,000 | |||
| 2010 | $1,612,745,000 | $1,650,253,000 | $1,620,494,000 | $1,636,371,000 |
| Rescission | $0 | |||
| 2011 | $1,681,333,000 | $1,678,696,000 | $1,636,371,000 | |
| Rescission | $14,368,312 | |||
| 2012 | $1,664,253,000 | $1,664,253,000 | $1,603,741,000 | $1,629,445,000 |
| Rescission | $3,079,651 | |||
| 2013 | $1,624,707,000 | $1,629,631,000 | $1,626,365,349 | |
| Rescission | $3,252,731 | |||
| Sequestration | ($81,632,357) | |||
| 2014 | $1,642,619,000 | $1,631,703,000 | $1,587,982,000 | |
| Rescission | $0 | |||
| 2015 | $1,608,461,000 | $1,605,205,000 | ||
| Rescission | $0 | |||
| 2016 | $1,660,375,000 | $1,656,758,000 | $1,694,758,000 | $1,696,139,000 |
| Rescission | $0 | |||
| 20171 | $1,695,180,000 | $1,751,049,000 | $1,803,306,000 | $1,696,139,000 |
| Rescission | $3,224,000 | |||
| 2018 | $1,355,998,000 | $1,853,011,000 | $1,904,666,000 | $1,783,654,000 |
| Rescission | $12,112,795 | |||
| 2019 | $1,838,556 |
1 Budget Estimates to Congress includes mandatory financing.
Justification of Budget Request
National Institute of Neurological Disorders and Stroke
Authorizing Legislation: Section 301 and Title IV of the Public Health Service Act, as amended.
Budget Authority (BA):
| FY 2017 Actual |
FY 2018 Annnnualized CR |
FY 2019 President's Budget |
FY 2019 +/- FY 2018 |
|
|---|---|---|---|---|
| BA | $1,778,688,000 | $1,771,541,206 | $1,838,556,000 | +$67,014,794 |
| F T E | 525 | 532 | 532 | 0 |
Program funds are allocated as follows: Competitive Grants/Cooperative Agreements; Contracts; Direct Federal/Intramural and Other.
Director's Overview
The National Institute of Neurological Disorders and Stroke (NINDS) supports research to improve the diagnosis, prevention, and treatment of disorders of the brain, spinal cord, and nerves of the body. Support for basic research on the normal nervous system and its diseases is especially crucial to building the foundation for public and private progress against disease. Chronic pain, Alzheimer’s disease related dementias (ADRDs), stroke, traumatic brain injury (TBI), epilepsy, Parkinson’s disease, multiple sclerosis, and other common neurological disorders affect millions of Americans of all ages. Hundreds of rare diseases add to the enormous impact. The multiplicity of diseases, the complexity of the brain, and the sensitivity of this remarkable organ to disruption of its indispensable functions present formidable challenges.
Despite these challenges, there is encouraging progress. In the past year, pioneering NIH-supported research and subsequent private sector development led to FDA approval of the first disease-modifying drugs for two rare pediatric diseases, spinal muscular atrophy (SMA) and Batten disease, and the first drug for primary progressive multiple sclerosis. Promising results have been reported for adrenoleukodystrophy, migraine, Niemann-Pick disease, and several other disorders. NINDS preclinical translational programs provide academic and small business investigators with milestone-driven funding, expert consultants, and contract resources to “de-risk” candidate drug, device, and biologic treatments to attract private sector investment or warrant NIH investment in further development. Therapies for migraine, familial dysautonomia, and Parkinson’s are among those moving forward in development.
Industry and NINDS agree that the development of biomarkers (measurable indicators) accelerates development of treatments for neurological disorders. The Parkinson’s Disease Biomarkers Program, TBI projects contributing to the Department-of-Defense-led TBI Endpoints Development program, and the Accelerating Medicines Partnership for Parkinson’s Disease (AMP PD) are among ongoing NINDS biomarkers activities. Development of biomarkers that will accelerate the development of non-addictive pain treatments is a high priority of the public private partnership among NIH, other agencies, and the private sector to address the opioid crisis.
Two decades ago, NINDS development of tPA therapy, which restores blood flow to the brain transformed emergency stroke care. In 2015, decades of NINDS and private research led to multiple clinical trials showing that intravascular devices can directly clear a blocked artery and provide striking clinical benefit in severe strokes when tPA does not restore blood flow. The NINDS DIFFUSE 3 clinical trial has now shown that brain imaging can identify people who may benefit well beyond the current restricted time window for this intervention. The NINDS StrokeNet Clinical Trials Network is continuing to conduct trials on treatment, as well as prevention and rehabilitation, as part of the Institute’s comprehensive clinical trials program.
NINDS clinical trials on stroke prevention contributed to the more than 70 percent decline in age-adjusted stroke death rates from 1968 to 20151. However, after more than four decades of steep decline, stroke death rates in the United States have fallen more slowly, stalled, or reversed among some population groups in recent years. Although the reasons are unclear, societal changes in risk factors, such as blood pressure control and obesity, especially in younger persons, may contribute. NINDS will continue to support research on stroke prevention, target persistent stroke disparities, and promote awareness of effective preventive measures. An update to the Institute’s comprehensive stroke planning will guide NINDS in confronting this challenge.
There is a growing understanding of the intersections between cerebrovascular disease and dementia. Stroke itself dramatically increases likelihood of developing dementia, and Vascular Cognitive Impairment and Dementia (VCID), which also involves brain blood vessels, is so intertwined with Alzheimer’s disease that most elderly people with dementia have a combination of the two. In the Framingham Heart Study, the dementia rate fell by 44 percent from the 1970’s to the 2010’s, and age of onset was delayed by five years2. The two leading explanations for this encouraging trend are improved vascular risk factor control and advanced levels of education. Congress, through the National Alzheimer’s Project Act (NAPA), recognized the impact of not just Alzheimer’s, but also ADRDs, which include frontotemporal dementia, the most common dementia before age 60, Lewy body and Parkinson’s dementias, in addition to VCID. NINDS leads NIH ADRD research and works with NIA to implement NAPA plans on ADRDs.
In response to an internal analysis, NINDS reinvigorated its support for basic research, the wellspring of progress. The Institute set aside funding to encourage fundamental research, led NIH to improve guidance for peer reviewers, and launched the Research Program Award, which provides outstanding investigators with freedom and sustained support to undertake ambitious, long-term projects. NINDS is also an enthusiastic leader of the Brain Research through Advancing Innovative Neurotechnologies (BRAIN) Initiative, which is developing tools that are revolutionizing basic research on how brain circuits work that will ultimately advance progress against the many neurological and psychiatric diseases that affect brain circuits. Pathological pain and addiction are classic disorders of brain circuits. NINDS will capitalize on the advances from the BRAIN Initiative to study these circuits and will also pursue the myriad of potential new drug targets revealed by NIH’s extensive investment in basic pain research more generally. Development of a clinical trials network for pain is another high priority of the public private partnership to address the opioid crisis.
Finally, to fulfil its mission NINDS must attract and sustain a vibrant and diverse scientific workforce. Neuroscience is a burgeoning field, perhaps more so than any other area of biomedical science, as reflected in the rising number of students in advanced training. For more than a decade, the Institute has aggressively supported early stage investigators. As for all aspects of its responsibilities, the Institute carefully monitors and analyses workforce trends and the effectiveness of its programs, and the results are encouraging. Thirty percent of NINDS principle investigators are now within the first five years after obtaining their first independent (R01) grant, and investigators in this early group receive a larger percentage of NINDS R01 funds than any other career stage. Fully half of NINDS investigators are within their first ten years of receiving an R01. NINDS continues a suite of programs to recruit and develop the best scientists and physicians from the full breadth of the nation’s talent pool, with programs that serve the needs of physician scientists, including neurosurgeons, and tailored programs and extensive outreach to promote diversity.
1 From Centers for Disease Control and Prevention MMWR September 8, 2017
2New England Journal of Medicine 374:523-32, 2016
Program Descriptions and Accomplishments:
The Institute continues to hold investigator-initiated research, with rigorous peer review, to be paramount because of its proven track record of driving progress. For more than a decade, NINDS has placed an especially high priority on supporting early stage investigators, including a substantial extension of the payline, and the Institute monitors its investments in research support across career stages. Likewise, NINDS has long placed a strong emphasis on maintaining robust support for basic research. This includes NINDS specific actions, such as the Research Program Award (R35) program, and leadership on this issue that led to NIH-wide actions, including instructions to peer reviewers and strong public statements by NIH leadership reinforcing the importance of basic research to the NIH mission. Complementing investigator-initiated research, the Institute solicits research proposals that target critical unmet public health needs or exceptional scientific opportunities, or provide common resources that enhance productivity of the research community. NINDS emphasizes good stewardship throughout its programs. To inform its decision making, the Institute monitors trends in research portfolios, evaluates specific programs, and engages stakeholders in strategic planning and in priority setting for specific diseases and issues. By scheduling interim analyses of large clinical trials and by monitoring milestones in large clinical studies and preclinical therapy development projects, NINDS shifts funds to the best current opportunities. Finally, NINDS has been among the leaders at NIH and in the scientific community in promoting transparency and reproducibility of research, which is essential to ensure the value of all research investments.
Channels, Synapses, and Circuits:Information flow in the nervous system occurs via circuits of neurons and interspersed glial (supporting) cells. Ion channels, synapses, and neural circuits are fundamental components of the nervous system. Ion channels control the electrical activity of cells. Synapses are specialized connections by which nerve cells influence the activity of other nerve cells. Circuits formed by networks of interconnected nerve cells carry out the information processing that enables us to perceive, think, and act. In addition to basic research on these fundamental components of the nervous system, the Channel, Synapses, and Neural Circuits Program supports studies on dysfunctions of channels, synapses, and circuits that underlie many neurological disorders. Epilepsy, a prime example, is a major focus of the program. Many types of epilepsy affect people of all ages. The causes of epilepsy include a host of newly discovered gene mutations, head injury, abnormal brain development, and other illnesses. Since 2000, the NINDS Epilepsy Benchmarks for Epilepsy Research have brought together disease advocates, the scientific community, and NIH to work toward the shared goal of curing all forms of epilepsy. Major priorities include improving treatment options for the one third of people with epilepsy do not respond well to any of the available treatments and understanding how epilepsy first develops with an eye toward informing the development of preventative treatments. This program also leads NINDS research on Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS), which is a poorly understood, complex, chronic condition that has a major impact on quality of life. NINDS chairs the Trans-NIH ME/CFS Working Group, which includes 24 Institutes and Centers, and funds research within the Institute’s realm of expertise. NINDS also directs an intramural research program on the Bethesda campus to understand the mechanisms underlying exertional exhaustion, muscle pain and fatigue, and to identify metabolic pathways and mediators of these pathways in men and women with ME/CFS.
In FY 2019, NINDS will continue to balance investigator-initiated research and research targeted to specific mission priorities, including projects funded through the Institute’s translational research and clinical trials programs. Among continuing research supported by initiatives, the Epilepsy Centers without Walls (CWOW) bring together the best multidisciplinary teams of investigators, regardless of geographic locations, to focus for multiple years on a specific Benchmarks priority that is better addressed through such a cooperative effort rather than traditional grant mechanisms. Areas of focus have included a very successful neurogenetics CWOW, a CWOW focusing on Sudden Unexpected Death in Epilepsy (SUDEP), and the a CWOW focused on finding treatments that modify the disease process itself and combating treatment resistant epilepsy. NINDS and NHLBI have also collaborated to expand the CDC’s Sudden Unexpected Infant Death (SUID) Case Registry to include SUDEP and Sudden Cardiac Death in individuals up to age 24 in 15 states. NINDS, along with other ICs, is promoting research on Myalgic Encephalitis/Chronic Fatigue Syndrome (ME/CFS) through support for Collaborative Research Centers that will work independently and collaboratively to define the causes of and develop improved treatments for ME/CFS.
Large Scale Clinical Research:The Division of Clinical Research (DCR) supports clinical trials infrastructure and directs large scale research programs, including early and advanced phase clinical trials and large epidemiological studies. DCR works closely with disease experts across all NINDS extramural programs. To optimize the efficiency and effectiveness of large scale clinical trials, DCR enforces milestones for progress, provides resources to improve patient access and recruitment, and supports multi-site clinical networks. DCR pioneered innovations for multi-site trials, including use of a single Institutional Review Boards, now adopted across NIH. The DCR Common Data Elements (CDE) Program works with the research and patient advocacy communities to develop standards for specific disorders that facilitate comparison and sharing of clinical data across studies, enhancing the value of these major clinical investments.
Developing a new clinical trials network to apply innovative study designs to accelerate biomarker informed testing of promising non-addictive pain medications is among NINDS’ highest priorities. This is an integral component of a multifaceted public private partnership among NIH, other agencies, and the private sector to address the opioid crisis. The continuing NeuroNEXT clinical network expedites early phase clinical studies across neurological disorders, including pediatric diseases, through central data and clinical coordinating centers and 25 clinical sites across the U.S. Two NeuroNext drug trials, one for progressive multiple sclerosis and one for acute stroke, were performed as part of a public private partnership and met their primary endpoints in 2017. In 2019, NINDS will continue to solicit proposals for NeuroNEXT pediatric and adult clinical studies from academic investigators, foundations, small businesses, and industry. The StrokeNet clinical trials network enhances the effectiveness of small and large stroke clinical trials by eliminating the costs and time associated with developing the infrastructure for each major trial anew and incorporating other efficiencies, such as central Institutional Review Boards and master contract agreements. The Network includes 25 regional clinical centers that work with 300 satellite clinical sites, as well as national clinical coordinating and data management centers. Studies on stroke prevention, acute treatment, and recovery are underway. The StrokeNet’s recently completed DEFUSE3 trial contributed to the radical change in emergency stroke care toward emergency endovascular treatment for severe ischemic stroke.
In FY 2018 the Institute will competitively renew the network and continue to seek clinical trial proposals from academic, industry, and small business investigators. The newest clinical network is a joint program with NHLBI. The Strategies to Innovate EmeRgENcy Care Clinical Trials Network (SIREN), launched in 2017, conducts multi-site clinical trials to improve the outcomes for patients with neurologic, cardiac, respiratory, and hematologic, and trauma emergency events. NINDS is also continuing its support for phase III investigator-initiated clinical trials across all neurological disorders, as well as major epidemiological studies that have contributed significantly to progress against stroke and other disorders.
Neural Environment:he circuits in the nervous system depend upon and are influenced by their local tissue environment, including the “neurovascular unit,” which controls the interface with the blood circulation. The Neural Environment Program supports basic research on the neurovascular unit and diseases in which its disruption plays a major role, and on translation of basic scientific knowledge into diagnostic tools, preventive measures, and targeted therapies. Non-nerve cells in the brain, called glial cells, together with specialized blood vessels and immune cells in the brain, maintain the local environment around nerve cells, fight infections, and control which molecules enter brain tissue from the circulating blood. These cells actively shape brain development and synapse function and are involved in a host of diseases, including Alzheimer’s, autism, and recovery from brain and spinal cord injury. Neurological disorders can result when non-neuronal cells are compromised; when these cells become aggressors in inflammatory or autoimmune disorders; when cells form tumors; when viruses, bacteria, or parasites infect the nervous system; or when the blood supply to brain cells is compromised, as in stroke. The Program also coordinates NINDS’ stroke activities, which span several parts of the Institute. NIH supported research on immunology of the brain and on glial cells has fostered private sector development of more than a dozen drugs for multiple sclerosis. Progress against brain tumors, another focus of this program, has been much more difficult to achieve, but a wide range of new studies are revealing potential strategies. For all diseases within the NINDS mission, the Institute coordinates closely with other components of NIH when our missions intersect; NINDS collaboration with NHLBI on stroke, NCI on cancer of the nervous system, and NIAID on multiple sclerosis and infectious diseases of the nervous system are among the many examples.
Neurodegeneration:The Neurodegeneration Program focuses on adult onset neurodegenerative diseases, in which brain cells progressively die. NINDS leads NIH research on Parkinson’s disease, Huntington’s disease, amyotrophic lateral sclerosis (ALS, or Lou Gehrig’s disease), and on ADRDs. The National Alzheimer’s Disease Project Act (NAPA) recognized the public health importance of related dementias that include vascular cognitive impairment/dementia (VCID), the second most common dementia, frontotemporal dementia (FTD), the most common dementia in people under 60 years old, and Lewy body dementia. Research has increasingly revealed connections among these neurodegenerative disorders, at every level of investigation from molecular mechanisms to risk factors. Among the unifying themes are the recognition that certain proteins form abnormal aggregates in many neurodegenerative disorders and that attention to genetic contributions can drive progress and reveal unsuspected connections, as that between ALS and FTD. Several drugs targeting steps in the underlying diseases revealed through genetic and molecular studies are now at various stages of testing.
NINDS neurodegeneration research will continue to balance investigator-initiated research and solicited research, including therapy development funded through the Institute’s translational research and clinical trials programs. The Institute is continuing to implement the Parkinson’s disease strategic plan. The NINDS Morris K. Udall Centers of Excellence for Parkinson’s Disease and the PD Biomarkers Program (PDBP) play an important role, as will the new Accelerating Medicines Partnership in Parkinson’s Disease (AMP PD). In 2016 NINDS led the 2016 Alzheimer’s Disease Related Dementias (ADRD) Summit which updated recommendations from a 2013 scientific conference on ADRD’s that were integrated into the National Alzheimer’s Project Act (NAPA) plan. Several new and ongoing NIH initiatives target priorities from the summit recommendations engaging expertise from multiple scientific and medical disciplines across all levels of analysis, from structural analysis of key proteins through epidemiological, though community-based studies of ADRDs in health disparities population.
Portrait of a Program: The Accelerating Medicines Partnership in Parkinson’s Disease (AMP PD)
The Accelerating Medicines Partnership (AMP) is a public-private partnership among NIH, the U.S. Food and Drug Administration (FDA), biopharmaceutical companies, and non-profit organizations. The overarching goal is to jointly accelerate the development of new therapeutics. AMP PD is a new partnership within the AMP program focused on Parkinson’s disease (PD). Following several workshops among the partners to identify key challenges and opportunities, unanimous agreement emerged that identifying and validating diagnostic, prognostic, and progression biomarkers for PD is the most promising avenue to accelerate progress against the disease. Biomarkers are measurable indicators of health, disease state, and therapeutic response. The availability of biomarkers will improve clinical trial design, matching of patients to appropriate interventions, monitoring of disease progression and treatment effectiveness, and identifying new pathways for therapy development.
AMP PD began in the fourth quarter of FY 2017 and will significantly expand in FY 2019 in accordance with a detailed implementation plan. The program builds on a strong foundation reflecting prior investments. Notably, the NINDS Parkinson’s Disease Biomarker Program (PDBP), the Michael J. Fox Foundation Parkinson’s Progression Makers Initiative (PPMI), and the Harvard NeuroDiscovery Center’s Biomarkers Discovery program together provide clinical, imaging, and genetic data and biosamples from 5,000 people with PD. After initial steps to harmonize datasets and establish the shared PD Knowledge Platform database, PD AMP will scale up to conduct multi-modal, large scale analyses for biological signatures of PD and its progression that may be further validated as biomarkers of PD and its progression, or point to promising new targets for development of treatments.
Gene defects cause hundreds of rare diseases that affect the nervous system, including ataxias, Down syndrome, dystonia, fragile X syndrome, lysosomal storage diseases, muscular dystrophies, peripheral neuropathies, Rett syndrome, spinal muscular atrophy, Tourette syndrome, and tuberous sclerosis, among many others. Genes also influence susceptibility to common neurological disorders. The Neurogenetics Program supports research on genes that cause or influence neurological disorders, molecular mechanisms by which these genes act, genetic animal and cell models of human disease, and development of treatments for neurogenetic disorders, from the laboratory to the clinic. Basic research to understand how genes and the environment orchestrate brain development is also a key aspect of the Neurogenetics Program. Research has identified hundreds of genes related to neurological disorders, which has led to tests that enable physicians to diagnose a disease months or even years more quickly than before, to animal models that provide insights about the underlying mechanisms of human diseases, and, most recently, the first disease modifying drugs for SMA (nusinersen), Batten disease (cerliponase alfa, and Duchenne muscular dystrophy (eteplirsen), with therapies for several other neurogenetic diseases as various stages of the development pipeline in the public and private sector.
NINDS will continue to support investigator-initiated grants and targeted activities in neurogenetics, including projects funded through the Institute’s translational research and clinical trials programs.
The Institute is providing substantial support for the application of whole genome sequencing and other “next generation” genomics methods to neurological disorders. Major continuing trans-NIH programs include the Paul D. Wellstone Muscular Dystrophy Cooperative Research Centers and the Autism Centers for Excellence. In 2015, the Muscular Dystrophy Coordinating Committee approved the updated Action Plan for the Muscular Dystrophies, which provides guidance not only for NIH activities in muscular dystrophy research, but also for other public and private entities. NINDS will continue to work closely with the NIH Office of Rare Disease Research in supporting and providing disease specific expertise to NINDS mission relevant consortia within the Rare Diseases Clinical Research Network. NINDS will also continue to support resources for neurogenetics research that enhance the efficiency and effectiveness of research by supporting sharing of data, biological samples, and research tools.
Repair and Plasticity:The Repair and Plasticity Program leads NINDS research on traumatic brain injury (TBI), spinal cord injury, and peripheral nerve injury. Research covers the full spectrum from injury to recovery, that is, from advancing understanding of the mechanisms of immediate damage and of the delayed effects in the hours after initial injury, through laboratory development of interventions that minimize damage or stimulate nervous system repair in animal models, to clinical testing in people. The Program also supports fundamental studies of neural plasticity, that is, the ability of the brain and nervous system to change, which has broad implications for recovery following injury or disease. This includes studies of stem cells in the brain. The Repair and Plasticity Program leads the longstanding NINDS Neural Interfaces Program, which pioneered technology for devices that connect to the nervous system to compensate for lost functions, including therapeutic brain stimulation technologies and brain computer interfaces that enable paralyzed people to control devices with their thoughts.
NINDS continues to balance investigator-initiated research and solicitations, including projects funded through the Institute’s translational research and clinical trials programs.
Large observational studies, now underway, are providing guidance to improve clinical care for TBI and clinical trials of interventions. These studies include the Transforming Research and Clinical Knowledge in TBI (TRACK TBI) study of adults and children with TBI at 11 sites in the U.S. and the Multiple Medical Therapies for Pediatric TBI (ADAPT Trial), which is focused on 1000 children with severe TBI. Both of these studies are part of the continuing International TBI Research Initiative in coordination with the European Union and the Canadian Institute of Health Research. These studies use the NINDS TBI Common Data Elements, developed with other Federal agencies and the international research community, and the NIH-Department of Defense led Federal Interagency TBI Informatics System (FITBIR) database to encourage sharing of data. With regard to the important public health issues of sports related TBI, NINDS is continuing to support research consortia to address the long-term consequences of mild and repetitive TBI, including chronic traumatic encephalopathy, which may appear years after exposure to impact. In 2019, the Neural Interfaces Program, will continue to solicit and support projects to translate advanced neural prosthetics and other devices up to and through “first in human” clinical demonstrations. NINDS supports device development through the Translational Neural Devices program, led by Repair and Plasticity together with the NINDS Division of Translation Research, which provides funding mechanisms tailored to the unique needs of device development at various stages and to the different FDA device approval pathways. The program is also working closely with the BRAIN Initiative in this promising area of research, including public-private partnerships with key device companies.
Systems and Cognitive Neuroscience:Systems of interconnected nerve circuits in the brain, spinal cord, and body control learning, memory, attention, language, thinking, emotion, sensation, movement, and response to pain, as well as sleep, feeding, and drinking. The Systems and Cognitive Neuroscience Program supports research on how the brain carries out these complex functions, on their disruption in neurological disorders, and on promoting recovery. Non-invasive brain imaging is an important research tool for this program, including monitoring of brain activity associated with specific types of thinking and behavior. NINDS is a partner in the Human Connectome Project, which has provided unparalleled data for neuroscientists on how parts of the brain interact with one another, creating maps of these connections called connectomes. Scientists are now building on the foundation of normal brain connectomes to examine how connectivity is altered through the lifespan and during disease. Chronic pain disorders, including migraine and other headaches, are among the most prevalent of all medical conditions. Pain research is among the highest priorities for NINDS, both because of the enormous impact of chronic pain itself and the role of the inadequacy of treatment options in driving the national opioid crisis. NINDS leads NIH pain research, which is coordinated through the Office of Pain Policy and the NIH Pain Consortium. The NINDS Office of Pain Policy manages the Interagency Pain Research Portfolio, a database that provides the public and the research community with information on the breadth and details of pain research and training activities supported by six Federal agencies.
NINDS balances investigator-initiated research and solicitations, including projects funded through the Institute’s translational research and clinical trials programs.
Pain continues to be a major area of emphasis, with NINDS coordinating NIH activities through the NIH Pain Consortium. The NINDS Office of Pain Policy, acting through the IPRCC led the development of the Federal Pain Research Strategy which was released in 2017. This plan, which is informed by the comprehensive Federal Pain Research Portfolio Analysis and International Pain Research Portfolio database, will guide pain research by the NIH Pain Consortium and by other agencies. As NIH lead for pain research, NINDS is intensively engaged with other parts of NIH, other agencies, and the private sector in a public private partnership to address the opioid crisis. NINDS expertise is especially crucial for the discovery and validation of biomarkers that will accelerate development of more effective non-addictive pain treatments and for development of a clinical trials network for pain research, noted above. The Institute is also continuing to support an extensive portfolio of basic research that is identifying potential targets for new pain agents and for interfering with the transition of normal, acute pain to abnormal, life-altering chronic pain.
Portrait of a Program: NIH Public-Private Partnerships to End the Opioid Crisis
As the lead Institute for pain research, NINDS recognizes the urgency of the opioid crisis and has special expertise to bring to bear. The Institute is working in concert with other components of the NIH, other Federal agencies, and the private sector. Intensive scientific workshops and discussions with the scientific community and industry partners from June through December 2017 were aimed at developing a partnership to enlist science to address the opioid crisis. The recommendations from these discussions included two key priorities, which NINDS is uniquely qualified to lead. Addressing these needs will accelerate the development of safe and effective, non-addictive treatments for pain, and thus reduce the reliance on opioids for the millions of people who suffer from chronic pain.
Basic research, largely supported by NIH, has identified many potential targets for new pain treatments. Industry has emphasized that a major barrier frustrating their efforts to capitalize on these opportunities is the lack of biomarkers. Biomarkers, that is, measurable indicators, quantify key factors, such as the extent to which a novel agent engages the intended molecular target in patients, which patients will respond to particular treatment strategies, and how effective a treatment actually is in r relieving pain. NINDS comprehensive program for such pain biomarker development will include all types of biomarkers and all stages of biomarker development, from early discovery, through optimization, and validation in multicenter clinical research.
The second, and interrelated initiative, is the development of a nation-wide Clinical Pain Research Network. The complex and heterogenous nature of the pain patient population presents unique challenges for academic and industry researchers attempting to find the appropriate patients for a particular clinical study. A single, comprehensive network will expedite recruitment of patients with numerous different pain conditions and enable industry and academic researchers to develop biomarkers and perform early stage drug testing on novel pain therapeutics at greater speed, reduced cost, and with greater confidence necessary to stimulate the considerable investment required. NINDS’ successful experience in pioneering innovative clinical trials networks for neurological disorders will enable the Institute to rapidly create an effective network for pain.
Training and Workforce Diversity: The Office of Training and Workforce Development, coordinates NINDS extramural programs for training and career development tailored to the specific needs of physicians and scientists at different stages of their careers, from pre-doctoral students onward. The Office of Programs to Enhance Neuroscience Workforce Diversity supports specific programs to enhance the diversity of the neuroscience workforce. All aspects of NINDS research depend on recruiting and supporting researchers from the full breadth of the nation’s talent pool, and both offices work closely with scientific staff across the institute to accomplish that. NINDS has redesigned its early stage training programs to improve opportunities for early-career neuroscientists and bolster their transition to independent research careers and is intent on lowering the age at which investigators start their independent research careers.
A full range of NINDS programs support training and career development. These include individual and institutional grants at the graduate, post-doctoral, and career development levels, and an intensive training course in clinical trials methods for fellows and faculty in the clinical neurosciences. Many of the programs target special needs, such as promoting diversity and enabling neurosurgeons to accommodate research preparation into their demanding training requirements. NINDS has redesigned its early stage training programs to improve opportunities for early-career neuroscientists and bolster their transition to independent research careers. These changes include a newly designed F32 postdoctoral fellowship program for early stage post-doctoral students, a new postdoctoral K01 program that enables advanced post-doctoral students to develop an independent research program, and a new NIH Blueprint predoctoral/postdoctoral (F99/K00) award to help recruit and retain faculty who represent the diverse make-up of our country. In FY 2018, NINDS initiated a new Mentor Award that recognizes the value of outstanding mentorship in developing each new generation of exceptional neuroscientists. In addition to dedicated training and career development programs, NINDS supports graduate students and post-doctoral researchers as investigators contributing their expertise on most research project grants in all of the Institute’s extramural and intramural programs.
Translational Research:The Division of Translational Research (DTR) leads NINDS preclinical therapy development activities for all diseases within the Institute’s mission. DTR supports the development of drugs, devices, and biologics, including cell and gene therapies. Successful projects may lead to further clinical development by NIH or “de-risk” the development path sufficiently to attract private sector handoff for further development. DTR preclinical therapy development experts work closely with disease-specific experts in extramural programs across the Institute and with the Division of Clinical Research to advance these interventions to first-in-human studies. The Innovation Grants to Nurture Initial Translational Efforts (IGNITE) Program provides a suite of funding opportunities for early stages of therapy development, for example, validation of assays to evaluate candidate drugs, demonstrations that proposed therapies have sufficient biological activity to warrant further development, and development of model systems for therapy development. Successful projects from IGNITE (or other promising research) progress into the Cooperative Research to Enable and Advance Translational Enterprises (CREATE) program for biologics (such as large biological molecules, gene therapies, and cell therapies) and the Translational Neural Devices program for devices. Together these funding mechanisms provide support from early stages through the development necessary to advance therapies into first in human studies. The Blueprint Neurotherapeutics Network supports the development of small molecule drugs. These advanced development programs gate funding based on rigorous milestones of progress and provide expert consultation and contract services that are often not readily available to academic investigators. The longstanding Epilepsy Therapy Screening Program (ETSP) provides resources for screening candidate drug therapies in standardized models and has contributed to the development of many of currently available drugs to treat epilepsy. DTR also coordinates all NINDS small business programs, which support innovative ideas at different stages of development, including applied bench research, translational research, and early stage clinical trials.
Intramural Research Program (IRP):IRP conducts research on the NIH campus in Bethesda, Maryland. The Program spans basic and translational neuroscience, neurology, and neurosurgery, and maintains its historical strengths in neuromuscular diseases, neurogenetics, neuroimmunology, membrane biochemistry and biophysics, and neurophysiology at the systems and synaptic level. The Mark O. Hatfield Clinical Center on the NIH campus in Bethesda, which is a hospital totally dedicated to clinical research, and the Porter Neuroscience Research Center, which integrates neuroscience across NIH ICs and disciplinary boundaries, provide unique resources to the Intramural Research Program. Ongoing basic research ranges from studies of individual molecules that control nerve cell behavior to advancing human brain imaging. Early phase clinical studies continue to be a strong aspect of the IRP, with studies now underway at the Clinical Center on Parkinson’s, epilepsy, multiple sclerosis, dystonia, neuropathies, and several other diseases, using drugs, invasive and noninvasive brain stimulation techniques, and gene therapy. The NINDS stroke research program studies patients with acute stroke and traumatic brain injury who present to two area emergency departments.
A national search is underway for a new IRP Scientific Director with the vision to build on the established strengths of the IRP and its unique resources, including the Clinical Center. The IRP will continue to make major contributions to national public health priorities, such as chronic fatigue syndrome/myalgic encephalitis, for which a clinical trial is underway, and TBI, though the Center for Neuroscience and Regenerative Medicine (CNRM), which is a collaboration with the Department of Defense, including the Walter Reed National Military Medical Center and the Uniformed Services University. CNRM, brings together clinicians and scientists across disciplines to catalyze innovative approaches to traumatic brain injury research.
Research Management and Support (RMS):RMS activities provide administrative, budgetary, logistical, and scientific support in the review, award, and monitoring of research grants, training awards, and research and development contracts. RMS functions also encompass strategic planning, coordination, and evaluation of the Institute’s programs, regulatory compliance, international coordination, and liaison with other Federal agencies, Congress, and the public.
Details of Full-Time Equivalent Employment (FTE's)
| OFFICE/DIVISION | FY 2017 Final |
FY 2018 Annualized CR |
FY 2019 President's Budget |
||||||
|---|---|---|---|---|---|---|---|---|---|
| Civilian | Military | Total | Civilian | Military | Total | Civilian | Military | Total | |
| Office of the Director | |||||||||
| Direct: | 1 | - | 1 | 1 | - | 1 | - | - | 1 |
| Reimbursable: | - | - | - | - | - | - | - | - | - |
| Total: | 1 | - | 1 | 1 | - | 1 | - | - | 1 |
| Office of the Director | |||||||||
| Direct: | 58 | - | 58 | 60 | - | 60 | 60 | - | 60 |
| Reimbursable: | - | - | - | - | - | - | - | - | - |
| Total: | 58 | - | 58 | 60 | - | 60 | 60 | - | 60 |
| Division of Clinical Research | |||||||||
| Direct: | 14 | - | 14 | 14 | - | 14 | 14 | - | 14 |
| Reimbursable: | - | - | - | - | - | - | - | - | - |
| Total: | 14 | - | 14 | 14 | - | 14 | 14 | - | 14 |
| Division of Translational Research | |||||||||
| Direct: | 19 | - | 19 | 17 | - | 17 | 17 | - | 17 |
| Reimbursable: | - | - | - | 1 | - | 1 | 1 | - | 1 |
| Total: | 19 | - | 19 | 18 | - | 18 | 18 | - | 18 |
| Division of Intramural Research | |||||||||
| Direct: | 305 | 6 | 311 | 307 | 6 | 313 | 307 | 6 | 313 |
| Reimbursable: | 14 | - | 14 | 16 | - | 16 | 16 | - | 16 |
| Total: | 319 | 6 | 325 | 323 | 6 | 329 | 323 | 6 | 329 |
| Division of Extramural Activities | |||||||||
| Direct: | 53 | - | 53 | 53 | - | 53 | 53 | - | 53 |
| Reimbursable: | - | - | - | - | - | - | - | - | - |
| Total: | 53 | - | 53 | 53 | - | 53 | 53 | - | 53 |
| Division of Neuroscience | |||||||||
| Direct: | 54 | - | 54 | 55 | - | 55 | 55 | - | 55 |
| Reimbursable: | 1 | - | 1 | 2 | - | 2 | 2 | - | 2 |
| Total: | 54 | - | 55 | 57 | - | 57 | 57 | - | 57 |
| Total | 511 | 9 | 520 | 524 | 8 | 532 | 524 | 8 | 532 |
Includes FTEs whose payroll obligations are supported by the NIH Common Fund.
FTEs supported by funds from Cooperative Research and Development Agreements.
| FISCAL YEAR | Average GS Grade |
|---|---|
| 2015 | 12.0 |
| 2016 | 12.3 |
| 2017 | 12.3 |
| 2018 | 12.5 |
| 2019 | 12.6 |
Detail of Positions3
(Dollars in Thousands)
| GRADE | FY 2017 Final Actual |
FY 2018 Annualized CR |
FY 2019 President's Budget |
|---|---|---|---|
| Total, ES Positions | 1 | 1 | 1 |
| Total, ES Salary | 187,000 | 190,550 | 191,450 |
| GM/GS-15 | 53 | 53 | 53 |
| GM/GS-14 | 53 | 53 | 53 |
| GM/GS-13 | 90 | 92 | 92 |
| GS-12 | 55 | 56 | 56 |
| GS-11 | 27 | 27 | 27 |
| GS-10 | 2 | 2 | 2 |
| GS-9 | 20 | 20 | 20 |
| GS-8 | 13 | 13 | 13 |
| GS-7 | 10 | 10 | 10 |
| GS-6 | 1 | 1 | 1 |
| GS-5 | 0 | 0 | 0 |
| GS-4 | 0 | 0 | 0 |
| GS-3 | 2 | 2 | 2 |
| GS-2 | 2 | 2 | 2 |
| GS-1 | 0 | 0 | 0 |
| Subtotal | 328 | 331 | 331 |
| Grades established by Act of July 1, 1944 (42 U.S.C. 207): | 0 | 0 | 0 |
| Assistant Surgeon General | 0 | 0 | 0 |
| Director Grade | 2 | 2 | 2 |
| Senior Grade | 1 | 1 | 1 |
| Full Grade | 2 | 2 | 2 |
| Senior Assistant Grade | 1 | 1 | 1 |
| Assistant Grade | 0 | 0 | 0 |
| Subtotal | 6 | 6 | 6 |
| Ungraded | 0 | 0 | 0 |
| Total permanent positions | 330 | 337 | 337 |
| Total positions, end of year | 534 | 541 | 541 |
| Total full-time equivalent (F T E) employment, end of year | 525 | 532 | 532 |
| Average ES salary | 187,000 | 190,550 | 191,450 |
| Average GM/GS grade | 12.3 | 12.5 | 12.6 |
| Average GM/GS salary | 109,141 | 111,215 | 111,743 |
3 Includes FTEs whose payroll obligations are supported by the NIH Common Fund.
