What is a spinal cord injury?
A spinal cord injury (SCI) is damage to the bundle of nerves and nerve fibers that sends and receives signals from the brain. The spinal cord extends from the lower part of the brain down through the lower back.
SCI can be caused by direct injury to the spinal cord itself or from damage to the tissue and bones (vertebrae) that surround the spinal cord. This damage can cause temporary or permanent changes in feeling, movement, strength, and body functions below the site of injury.
Symptoms
The symptoms of spinal cord injuries depend on the extent and location of the injury. The higher up on the spinal cord an injury occurs, more of the body is affected. An injury higher on the spinal cord can cause paralysis in most of the body and affect all limbs (tetraplegia or quadriplegia). An injury that occurs lower down the spinal cord may only affect a person’s lower body and legs (paraplegia). Paralysis can happen immediately upon injury (primary damage) or develop over time from bleeding and swelling in the spinal cord and cell death (secondary damage).
A spinal cord injury can damage a few, many, or almost all of the nerve fibers that cross the site of injury. If the injury causes little or no nerve cell death, a person can make an almost complete recovery.
SCI can cause one or more symptoms, including:
Types of SCI
SCI can be described as complete or incomplete.
- An incomplete injury means the spinal cord is still able to send some messages to or from the brain. People with incomplete injuries still have some feeling, function, and muscle control below the site of their injury.
- A complete injury means that there is no nerve communication below the injury site; muscle control, feeling, or function below the injury is lost.
Anatomy of the spinal cord
The spinal cord is a soft, cylindrical column of tightly bundled cells (nerve cells and glia), nerve fibers that transmit nerve signals (called axons), and blood vessels. It sends and receives information between the brain and the rest of the body. Millions of nerve cells situated in the spinal cord itself coordinate complex patterns of movements such as rhythmic breathing and walking.
The spinal cord extends from the brain to the lower back through a canal in the center of the vertebrae. Like the brain, the spinal cord is protected by three layers of tissue and is surrounded by the cerebrospinal fluid (CSF) that acts as a cushion against shock or injury.
Inside the spinal cord are:
- A collection of nerve cells and their projections that connect with other nerve cells to transmit and receive information (gray matter)
- Bundles of nerve fibers (axons), some of which are coated with a whitish mixture of proteins and fat-like substances (white matter) that connects nerve cells over longer distances.
Other types of nerve cells sit just outside the spinal cord and relay information to and from the brain.
- Cervical spinal nerves (known as C1 to C7) in the neck control signals to the back of the head, the neck and shoulders, the arms and hands, and the diaphragm.
- Thoracic spinal nerves (known as T1 to T12) in the upper mid-back control signals to the chest muscles, some muscles of the back, and many organ systems.
- Lumbar spinal nerves (known L1 to L5) in the low back control signals to the lower parts of the abdomen and the back, the buttocks, some parts of the external genital organs, and parts of the leg.
- Sacral spinal nerves (known S1 to S5) in the low back control signals to the thighs and lower parts of the legs, the feet, most of the external genital organs, and the area around the anus.
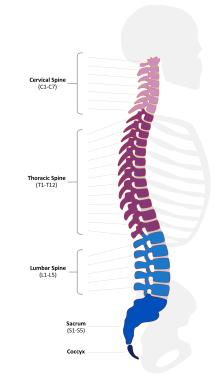
The spinal column, which surrounds and protects the spinal cord, is made up of 33 rings of bone (vertebrae), pads of cartilage (discs), and narrow spaces called foramen that act as passages for spinal nerves to travel to and from the rest of the body. The spinal cord is particularly vulnerable to direct injury within the foramen.
Who is more likely to get a spinal cord injury?
Motor vehicle accidents and serious falls are the most common causes of SCI in the U.S. Other causes include acts of violence (primarily gunshot wounds and assaults), sports injuries, medical or surgical injury, industrial accidents, diseases, and conditions that can damage the spinal cord. Risk factors include age (either being between the ages of 16 and 30, or after age 65 for dangerous falls), alcohol use, certain diseases, or not wearing proper gear, such as a seat belt or protective sports equipment.
How is a spinal cord injury diagnosed and treated?
Diagnosing SCI
The emergency room physician will check for movement or sensation at or below a suspected SCI, as well as for proper breathing, responsiveness, and weakness. Medical tests for SCI include:
- Magnetic resonance imaging (MRI) can show brain and spinal trauma from injury, herniated discs (problems with the cartilage located between the vertebrae), vascular (blood vessel) irregularities, bleeding, inflammation that might compress the spine and spinal cord, and injury to the ligaments that support the cervical spine.
- Computerized tomography (CT) can detect bone fractures, bleeding, and spinal stenosis (narrowing of the spinal canal).
- X-rays can show vertebrae misalignment and fractures within minutes of injury.
Treating SCI
At the accident scene, if SCI is suspected, emergency personnel will place a rigid collar around the neck and carefully place the individual on a backboard to prevent further damage to the spinal cord. They may use sedatives to relax the person and prevent movement. A breathing tube may be inserted if there are problems breathing and the body isn't receiving enough oxygen from the lungs.
Doctors are now able to predict with reasonable accuracy the likely long-term outcome of SCI. This helps people experiencing SCI to set achievable goals for themselves and gives families and loved ones a realistic set of expectations for the future.
Immediate treatment at the trauma center or emergency room may include:
- Realigning the spine using a rigid brace or mechanical force, which is usually done as soon as possible to stabilize the spine and prevent additional damage.
- Surgery to remove any fractured vertebrae, bone fragments, herniated discs, or other objects that are pressing on the spinal column. Spinal decompression surgery to relieve pressure within the spinal column may also be necessary in the days after injury. Results of neurosurgical studies show that, in some cases, earlier surgery is associated with better functional recovery.
SCI may result in the following problems, which require treatment:
- Breathing problems—About one-third of people with a SCI will need temporary or permanent help with breathing and may require a breathing tube. Any injury to the spinal cord between the C1-C4 segments can stop breathing as the nerves in this region cause the diaphragm to move and the lungs to expand. Special training regarding breathing and swallowing may be needed for the individual with SCI as well as for the caregivers.
- Pneumonia—Respiratory complications are the leading cause of death in people with SCI, commonly as a result of pneumonia. Individuals using a ventilator to assist with breathing (intubation), are at increased risk of developing pneumonia. The person with a SCI must be carefully monitored and treated with antibiotics if symptoms of pneumonia appear. Pneumonia can be prevented by clearing the throat and taking precautions to avoid food and liquids being sucked into the lungs (aspiration).
- Circulatory problems—Changes in circulation can lead to unstable blood pressure, abnormal heart rhythms (arrhythmias), and blood clots that may appear days after injury. The injured person should be carefully monitored for each of these common post-SCI issues. People with spinal cord injuries are at increased risk for blood clots due to stagnation of blood flow in the large veins in the legs. Anticoagulant drugs and compression stockings to increase blood flow in the lower legs and feet and reduce the risk for blood clots.
- Stiffness and changes in muscle tone—Reflexes may become exaggerated over time, causing muscle stiffness and an increase in muscle tone (spasticity) that may require special treatment. Muscles below the injury site may deteriorate when they are not used.
- Autonomic dysreflexia—Autonomic dysreflexia is a life-threatening reflex action that primarily affects those with injuries to the neck or upper back. Symptoms may include flushing or sweating, a pounding headache, anxiety, sudden increase in blood pressure, vision changes, or goose bumps on the arms and legs. If possible, the person should be kept in a sitting position to keep blood flowing to the legs and feet and help reduce blood pressure.
- Pressure sores (also known as pressure ulcers)—Pressure sores are areas of skin that have broken down because of continuous pressure on the skin and reduced blood flow to the area. People with paraplegia and tetraplegia are susceptible to pressure sores. As a result, individuals must move and change their position periodically, either on their own or with the help of assistive devices or a caregiver.
- Pain—Some people with SCI develop neurogenic pain—an intense burning or stinging sensation. This pain may be constant or may come and go. It can be triggered by a variety of factors and may even be felt in parts of the body that have otherwise lost sensation. Treatments for chronic pain include medications, acupuncture, spinal or brain electrical stimulation, and surgery. However, none of these treatments are completely effective at relieving neurogenic pain long term.
- Bladder and bowel problems—Individuals may need to use a catheter to empty their bladder and learn new ways to empty the bowels. The person may need to change their diet.
- Sexual function—Depending on the severity and location of the injury, and the individual’s recovery after the injury, their sexual function and fertility may be affected. A urologist and other specialists can suggest different options to support sexual functioning and health.
- Depression—Many people living with SCI may develop depression due to lifestyle changes after the injury. Therapy and medicine can help treat depression and other mental health conditions.
Rehabilitation
Rehabilitation programs for people with SCI combine physical therapies with skill-building activities and counseling designed to provide social and emotional support and increase the person’s independence and quality of life. The rehabilitation team is usually led by a doctor specializing in physical medicine and rehabilitation and may include social workers, physical and occupational therapists, recreational therapists, rehabilitation nurses, rehabilitation psychologists, vocational counselors, nutritionists, a case worker, and other specialists.
The initial phase of rehabilitation after injury is usually focused on regaining communication skills and leg and arm strength. Adaptive or assistive devices may help people with SCI to regain independence and improve mobility and quality of life. Depending on the severity of the injury, the person may need braces, a wheelchair, electronic stimulators, assisted training with walking, neural prosthetics (assistive devices that may stimulate the nerves to restore lost functions), computer adaptations, and other computer-assisted technology. Adaptive devices can also help with communication skills such as writing, typing, and using the telephone.
- Physical therapy includes exercise programs geared toward strengthening muscles.
- Occupational therapy helps redevelop fine motor skills, particularly those needed to perform activities of daily living such as getting in and out of a bed, personal hygiene, eating, and using the toilet. The person may learn how to cope with spasticity, autonomic dysreflexia, and neurogenic pain as part of their occupational therapy.
- Vocational rehabilitation includes identifying basic work skills and physical and cognitive capabilities that can support paid work. Through this process, the person and their team can identify potential workplaces and any assistive equipment that will be needed and arrange for a user-friendly workplace.
- Educational training can help the person develop skills for a new line of work that may be less dependent upon a person’s physical abilities. People with SCI are encouraged to participate in activities that provide a sense of satisfaction and self-esteem, such as educational classes, hobbies, special interest groups, and participating in family and community events.
- Recreation therapy encourages people with SCI to participate in sports, arts, or other leisure activities that they can do with their new level of mobility. This can help people achieve a balanced lifestyle that provides opportunities for socialization and self-expression.
What are the latest updates on spinal cord injury?
NINDS, a component of NIH, is a primary funder of research on the brain and spinal cord. NIH is the leading supporter of biomedical research in the world.
NINDS investment in establishing the field of neural devices has supported significant advances with potential to improve post-injury quality of life for people with SCI. For example, researchers are developing an electrical stimulation system that is used as a network to restore functional independence through combined implants for hand function, postural control, and bowel and bladder control. Other research involves stimulating the spinal cord below the level of injury to help spared cells and fibers function. NINDS has also led development of experimental brain computer interfaces that enable people to control a computer cursor or robotic arm directly from their brains.
Current research on SCI is focused on advancing our understanding of the four key principles of spinal cord repair:
- Neuroprotection—Preventing cell death and protecting surviving nerve cells from further damage, including using drugs to reduce nerve cell death and lowering of the body's core temperature to reduce damage and improve functional outcome.
- Repair and regeneration—Encouraging the spinal cord to self-repair and stimulating the regrowth of nerve fibers. These efforts include exploring cell transplants, growth-promoting substances, and bioengineered growth scaffolds.
- Cell-based therapies—Replacing damaged nerve or support cells with other cell types, including stem cells, to jumpstart nerve cell growth and create new cell connections.
- Neuroplasticity—Retraining central nervous system circuits to restore body functions and form new nerve connections and pathways following injury or cell death through techniques like rehabilitation, electrical stimulation, robot-assisted training, and brain-computer interface technology that may help with voluntary muscle movement and coordination.
Further research includes basic spinal cord function studies on how the spinal cord develops, processes sensory information, controls movement, and generates rhythmic patterns like walking and breathing. Studies using cells and animal models provide an essential foundation for developing interventions for spinal cord injury. And research on injury mechanisms focuses on what causes immediate harm and on the cascade of reactions the body deploys that protect from (or contribute to) secondary damage in the hours and days following a SCI This includes testing neuroprotective interventions in animal models.
The Brain Research through Advancing Innovative Technologies® (BRAIN) Initiative brings multiple federal agencies and private organizations together to develop and apply new technologies to understand how complex circuits of nerve cells enable thinking, movement control, and perception. BRAIN’s SCI research includes:
- Exploring brain circuits to better understand the sensory and motor basis of behavior
- Next-generation neural prosthetics, or devices that connect to the nervous system and restore functions lost due to disease or injury
- Improved brain and spinal cord imaging
- New brain-computer interface devices
NINDS also has developed Common Data Elements (CDEs) for SCI. CDEs are critical to ensure that data from clinical studies is collected and reported in a consistent way.
More information about SCI research may be found using NIH RePORTER, a searchable database of current and past research projects supported by NIH and other federal agencies. RePORTER also includes links to publications and resources from these projects.
For research articles and summaries on SCI, search PubMed, which contains citations from medical journals and other sites.
How can I or my loved one help improve care for people with a spinal cord injury?
Consider participating in a clinical trial so clinicians and scientists can learn more about SCI. Clinical research uses human study participants to help researchers learn more about a disorder and perhaps find better ways to safely detect, treat, or prevent disease.
All types of study participants are needed—those who are healthy or may have an illness or disease—of all different ages, sexes, races, and ethnicities to ensure that study results apply to as many people as possible, and that treatments will be safe and effective for everyone who will use them.
For information about participating in clinical research visit NIH Clinical Research Trials and You. Learn about clinical trials currently looking for people with SCI at Clinicaltrials.gov, a searchable database of clinical trials.
Spinal cord injury and rehabilitation research centers maintain registries of people interested in participating in ongoing or future clinical studies. A multi-site network supported by the Christopher and Dana Reeve Foundation called the NeuroRecovery Network (NRN) accepts volunteer research participants. Signing up for the registry does not obligate a person to participate in a study. Registries are designed to help gather a list of potential participants that can be consulted as studies are initiated.
