If you have neurological symptoms like headaches, sleep problems, or memory loss, there are several tests and procedures your doctor may do to find out if you have a brain disorder or another medical condition. While some brain disorders can be hard to diagnose, research has advanced our ability to detect—and treat—many neurological disorders and related conditions. This article has information about common tests and procedures doctors use to diagnose neurological disorders.
One hundred years ago, the only way to make a definite diagnosis for many neurological disorders was to do an autopsy after the person had died. Today, new instruments and techniques allow scientists to assess the living brain and monitor nervous system activity as it happens. Doctors now have powerful and accurate tools to better diagnose disease and to test how well a specific treatment may be working.
Researchers and physicians use imaging techniques and blood and cerebrospinal fluid tests to detect, manage, and treat brain disorders. Many tests can be done in a physician’s office or at an outpatient testing facility, with little or no risk. Some procedures are done in specialized settings, such as a hospital.
Perhaps the most significant changes during the past 10 years have happened in genetic testing and diagnostic imaging. Scientists have learned a lot from sequencing the human genome (the complete set of a person’s genes) and developing new technologies that detect genetic mutations. Improved imaging techniques create high resolution images that allow physicians to view the structure of the brain. Specialized imaging methods can show changes in brain activity or in certain brain chemicals. Scientists continue to improve these methods to provide more detailed diagnostic information.
What is a neurological examination?
You may need a neurological examination if you have symptoms that include the following:
You may also need a neurological exam if you have had an injury that may have damaged your peripheral nerves, spinal cord, or brain (such as a traumatic brain injury or TBI).
Levi's Story
Levi, age 14, got hit in the head with a soccer ball during a match. His coach was concerned that Levi experienced a concussion and had him sit out the rest of the game. The coach then recommended that Levi’s parents take him to see his doctor as soon as possible. During the appointment, the doctor asked Levi how he was feeling and checked around his head where he got hit. She then tested things like Levi’s memory, reflexes, and blood pressure to get a better picture of his condition. After reviewing his assessment results and medical history, the doctor determined that Levi didn’t have a concussion—but she still recommended he rest for a few days to be safe.
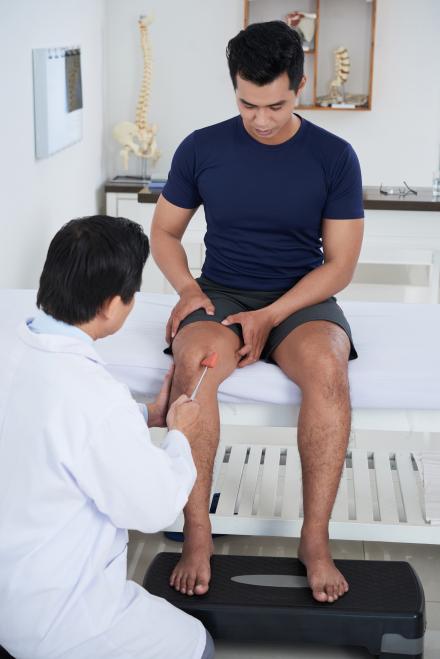
What happens during a neurological examination?
Next, the provider will do specific tests to check how different parts of your nervous system are working. The tests you have will depend on your symptoms. The examination may include tools such as a tuning fork (to test for hearing loss and as part of a sensory exam), flashlight, or a reflex hammer. The tests may check your:
- Mental status. This includes your memory, problem-solving ability, alertness, and mood. During a mental status exam, you may answer questions about the date, time, and where you are. You may also be asked to remember a list of items, name objects, repeat words, and/or draw specific shapes.
- Cranial nerves. These 12 nerves connect your brain with your eyes, ears, nose, face, tongue, throat, shoulders, and certain organs. The provider will test the nerves that may be involved with your symptoms. For example, to test your sight, you may be asked to read a letter chart. To test the muscles in your face, you may be asked to smile or close your eyes tightly.
- Movement and strength. Muscles respond to signals from the brain and nervous system and can help doctors identify problems with the brain and spinal cord. During a neurological examination, doctors will test the strength and flexibility of your muscles. You may be asked to keep your fingers spread apart while the provider gently pushes them together, or to relax your arm while they move it back and forth.
- Coordination, balance, and walking. These tests check how well your nervous system controls your muscle movements. You may be asked to walk in a straight line placing one foot directly in front of the other. Other tests include checking your handwriting and having you touch your finger to your nose with your eyes closed.
- Reflexes. A reflex is your body's automatic movement in response to certain triggers. For example, if your knee is tapped with a rubber hammer, your lower leg will jerk on its own. There are many types of reflexes that are tested in different ways. Reflex tests show how well nerves that send signals between your spinal cord and muscles are working.
- Sensory nerves. The doctor may test how well you can feel touch, hot and cold temperatures, vibrations, and pain. These tests involve gently touching parts of your skin with different objects, such as a sharp object or a cotton swab. You will be asked to describe what you can feel.
- Autonomic nervous system. A neurological exam tests the part of your nervous system that controls your breathing, heart rate, digestion, and other processes that happen without thinking. Examples of these tests include checking your blood pressure and heartbeat.
In infants and young children, many of these parts of the exam are based on observation or engagement in play activities.
The results of the neurological examination and the person’s history help determine a list of possibilities, known as the differential diagnosis, that determine if more diagnostic tests and procedures are needed.
If the results of any part of your neurological exam are not normal, your doctor will probably order more tests to help make a diagnosis. These screening tests will depend on what type of condition your doctor thinks you may have.
What are some common screening tests?
Laboratory tests
Laboratory tests of blood, urine, or other body fluids may help doctors diagnose disease or understand disease severity. These tests can also help monitor levels of medications in the body to help determine if the person is taking the right dose. Certain tests, ordered by the physician as part of a regular checkup, give general information, while others can identify specific health concerns:
- Blood tests can detect infections, toxins, clotting disorders, or antibodies that show the presence of an autoimmune disease. They can also monitor levels of drugs that treat epilepsy and other neurological disorders in the body.
- Genetic testing of DNA extracted from cells in the blood or saliva can help diagnose hereditary disorders
- Analysis of cerebrospinal fluid (the fluid that surrounds the brain and spinal cord) can detect meningitis, encephalitis, acute and chronic inflammation, viral infections, multiple sclerosis, and certain neurodegenerative disorders
- Chemical and metabolic testing of the blood can point to some muscle disorders, protein or fat-related disorders that affect the brain, and metabolic problems
- Urine tests can reveal toxins, abnormal metabolic substances, proteins that cause disease, or signs of certain infections
Genetic testing
Genetic testing of people with or without a family history of a neurological disease can determine if they are carrying one of the genes known to cause the disorder. Genetic counseling may help people understand the purpose of the tests and what the results could mean. Genetic testing for diagnosis or treatment should be done in a laboratory that has been certified for clinical testing. Clinical testing can look for disease-causing mutations in specific genes or in regions of several genes. This testing may use a panel of genes for a specific type of disease (for example, infant-onset epilepsy) or a test known as whole exome sequencing. Exomes are the parts of the genome formed by exons, which code for proteins. Whole genome sequencing is also now used in certain cases. Exome and genome sequencing may take several months to analyze. Clinicians and researchers also sequence whole exomes or whole genomes to discover new genes that cause neurological disorders.
Prenatal genetic testing can identify many neurological disorders and genetic abnormalities before birth.
- A pregnant person’s blood can be screened for abnormalities that suggest a risk for a genetic disorder.
- A type of blood test called a quadruple or quad screen may help identify some genetic disorders, including trisomies (which cause disorders such as Down syndrome) in a fetus. A blood sample measures the levels of four substances: alpha-fetoprotein, human chorionic gonadotropin, estriol, and inhibin-A. The test is done between 15 and 20 weeks of pregnancy. It usually takes several days to receive results from a quad screen. Abnormal results of a quad screen may point to spina bifida or a chromosome abnormality. However, false positive results are not uncommon, so more testing may be needed.
- Amniocentesis is usually done at 14-16 weeks of pregnancy if there is a suspected problem with the fetus. It tests a sample of the amniotic fluid in the womb for genetic defects. Under local anesthesia (anesthesia that is given while you are awake for a short time to stop pain in one part of the body), a thin needle is inserted through the abdomen and into the womb. About 20 milliliters of fluid (roughly 4 teaspoons) is withdrawn and sent to a lab for evaluation. Test results often take 1-2 weeks.
- Chorionic villus sampling is done at 10-13 weeks of pregnancy. The procedure removes and tests a very small sample of the placenta. The sample, which contains the same DNA as the fetus, is taken out by catheter or fine needle inserted through the cervix or by a fine needle inserted through the abdomen. Chorionic villus sampling is usually only done if there is a high risk of a genetic abnormality, for example, if the mother is age 35 or older or one of the parents has a family history of a genetic condition. Results are usually available within 2 weeks.
Visit the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) to learn more.
Brain scans
Brain scans include several types of imaging techniques that diagnose tumors, blood vessel malformations, stroke, inflammation, injuries, scars, abnormal brain development, and hemorrhage in the brain. Types of brain scans include CT (computed tomography), MRI (magnetic resonance imaging), PET (positron emission tomography), and SPECT (single proton emission CT). The type of scan that will be recommended depends on the results of the neurological exam and the person’s symptoms. Brain scans are done by skilled technicians in a hospital or at an outpatient testing facility.
Computed tomography (CT scan)
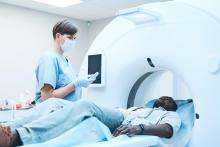
Computed tomography (CT scan) uses X-rays to produce two- and three-dimensional images of organs, bones, and tissues. A CT scan can aid in proper diagnosis by showing the area of the brain that is affected. CT scans can quickly detect bleeding in the brain and determine if someone who has had a stroke can safely receive IV treatment to dissolve clots. CT scans can also help detect bone and blood vessel irregularities, brain tumors and cysts, hydrocephalus (build-up of cerebrospinal fluid in the brain), or brain damage from an injury. A CT of the spine can show herniated discs, spine fractures, or spinal stenosis.
CT scans are especially useful in people who can’t have an MRI. Because CT uses X-rays, pregnant people have them only under limited circumstances (typically, emergencies) because of potential harm to the fetus.
During a CT scan:
- CT scanning takes about 20 minutes and is usually done at an outpatient imaging center or in a hospital.
- The person lies on a special table that slides into a narrow, doughnut-shaped chamber.
- A sound system built into the chamber allows the person to communicate with the physician or technician. X-rays (ionizing radiation) are passed through the body at various angles and are detected by a computerized scanner.
- The data is processed and displayed as cross-sectional images, or “slices,” of the internal structure of the body or organ.
- Occasionally, a light sedative may be given if the person is unable to lie still. Pillows can support and stabilize the head and body.
- Sometimes, a contrast dye is injected into the bloodstream to highlight the different tissues in the brain. If a contrast dye is injected into a vein, the person being scanned may feel a warm or cool sensation as the dye circulates through the bloodstream or may experience a slight metallic taste.
Magnetic resonance imaging (MRI)
Magnetic resonance imaging (MRI) uses computer-generated radio waves and a powerful magnetic field to produce detailed images of body tissues. Using different sequences of magnetic pulses, MRI can show images of the brain or spinal cord, measure blood flow, or reveal deposits of minerals such as iron. MRI can help diagnose stroke, traumatic brain injury, brain and spinal cord tumors, inflammation, infection, vascular problems, scars, abnormally developed brain regions, and some neurodegenerative disorders. MRI can also help diagnose and monitor multiple sclerosis.
The test is painless and risk-free, although people with obesity or people who are claustrophobic may find it somewhat uncomfortable—the machine can also be noisy. Some centers use open MRI machines that do not completely surround the person being tested and are less confining. However, open MRI does not currently provide the same picture quality as standard MRI.
During an MRI:
- A contrast dye may be injected into the vein to better show certain areas or tissues. If intravenous contrast is required, people may first need a blood test to check kidney function because the contrast agent, called gadolinium, can increase the risk of a rare disease in people with advanced kidney disease.
- An MRI scanner has a tube surrounded by a very large cylinder-shaped magnet.
- The person lies on a special table that slides into the tube and will be asked to remove jewelry, eyeglasses, removable dental devices, clothing with metal, and other items that might interfere with the magnetic imaging. Because people must remain still during the MRI, very young children (or those with certain medical conditions) may need to be sedated to be scanned.
- For brain MRI scans, a detector is placed over the head.
- The person may hear grating or knocking noises when the magnetic field direction is flipped. Earphones or earplugs can help block out the sounds.
- MRI scanners create a magnetic field around the body that’s strong enough to temporarily realign water molecules in the tissues. Radio waves are then passed through the body to detect the shifting of molecules back to a random order.
- A computer then reconstructs a three-dimensional picture or a two-dimensional “slice” of the tissue being scanned.
- MRI can tell the difference between bone, soft tissues, and fluid-filled spaces because of differences in water content and tissue properties.
- Depending on the part(s) of the body to be scanned, MRI can take up to an hour to complete.
Due to the incredibly strong magnetic field generated by an MRI, people with implanted medical devices such as a pacemaker or infusion device generally should not have MRIs. In certain situations, facilities may have equipment to temporarily stop and reset the implanted device’s programming to allow the person to receive an MRI. A fetal MRI may be ordered when prenatal ultrasound reveals a possible problem. Fetal MRI is considered safe for the fetus because it doesn’t use radiation or contrast dye.
Functional MRI (fMRI)
Functional MRI (fMRI) uses the blood’s magnetic properties to create real-time images of blood flow to specific areas of the brain. fMRI can pinpoint areas of the brain that become active and show how long they stay active. This imaging process can help identify brain regions that are critical for language, motor function, or sensation before surgery for epilepsy. Researchers use fMRI to study head injury and degenerative disorders such as Alzheimer’s disease.
Positron emission tomography (PET)
Positron emission tomography (PET) scans create two- and three-dimensional pictures of brain activity by measuring radioactive isotopes that are injected into the bloodstream. PET scans of the brain can detect or highlight tumors and diseased tissue, show blood flow, and measure cellular and/or tissue metabolism. PET scans can evaluate people who have epilepsy or certain memory disorders and show brain changes following injury. PET may be ordered as a follow-up to a CT or MRI scan to give the physician a greater understanding of activity in specific areas of the brain.
During a PET scan:
- A low-level radioactive isotope, also called a tracer, is injected into the bloodstream. The PET scan measures where tracer goes in the brain.
- The person lies still while overhead sensors detect gamma rays in the body’s tissues.
- A computer processes the information and displays it on a video monitor or on film.
- Using tracers, more than one brain function can be traced at the same time.
- PET is painless and uses small amounts of radioactivity.
- The length of test time depends on the part of the body to be scanned.
Single photon emission computed tomography (SPECT)
Single photon emission computed tomography (SPECT) is a nuclear imaging test that can evaluate certain brain functions. As with a PET scan, a tracer is injected into the body. A SPECT scan may be ordered as a follow-up to an MRI to diagnose tumors, infections, brain regions involved in seizures, degenerative spine disease, and stress fractures.
During a SPECT scan:
- The person lies on a table while a gamma camera rotates around the head and records where the tracer has traveled.
- That information is converted by computer into cross-sectional slices that are stacked to produce a detailed three-dimensional image of the tracer within the brain.
A person who experiences a seizure can get two scans after they’re medically stable—one as an initial baseline scan and after a tracer is injected.
A dopamine transport single-photon emission computed tomography scan (DaTscan) can help diagnose Parkinson’s disease.
Lisa's Story
Lisa, age 30, had been feeling some stiffness in her muscles and dizziness. She often found it difficult to stay balanced while walking. Lisa scheduled an appointment with her doctor, who performed a physical exam. The doctor referred her to a neurologist for an MRI (magnetic resonance imaging) scan based on her symptoms. The MRI results showed signs of multiple sclerosis. They prescribed Lisa medicines to help with her symptoms and recommended lifestyle changes.
What additional tests are used to diagnose neurological disorders?
The following list of procedures—in alphabetical order—describes some of the other, less common tests used to help diagnose neurological conditions. Doctors use some of these tests because they can show certain issues that they can't see with more common screening tests, such as a CT scan or MRI.
Angiography
Angiography involves injecting dye into the arteries or veins to detect blockage or narrowing. A cerebral angiogram can show narrowing or obstruction of an artery or blood vessel in the brain, head, or neck. It can determine the location and size of an aneurysm or vascular malformation. Angiograms are used in certain strokes where there is a possibility of unblocking the artery using a clot retriever. A spinal angiogram can help detect problems in the spinal cord blood vessels—such as malformations or blockages in arteries. Angiograms can also show the blood supply of a tumor before an operation and are usually done in a hospital or at an outpatient testing facility.
During an angiogram:
- The person lies on a table that is wheeled into the imaging area.
- A physician numbs a small area of the leg near the groin and then inserts a catheter into a major artery located there.
- They then thread the catheter through the body and into an artery in the neck.
- The technician injects a dye that travels through the bloodstream into the head and neck and takes a series of X-rays. The person may feel a warm to hot sensation or slight discomfort as the dye is released.
- This may take up to 3 hours, followed by a 6- to 8-hour resting period.
In many situations, brain angiograms have been replaced by specialized MRI scans, called MR angiograms (MRA), or CT angiograms.
Biopsy
Biopsy involves the removal and examination of a small piece of tissue from the body. Muscle or nerve biopsies can help diagnose neuromuscular disorders. A skin biopsy can measure small nerve fibers or test for certain metabolic disorders.
They are usually done in an outpatient testing facility.
During a biopsy:
- A small sample of the muscle, skin, or nerve is removed under local anesthetic.
- The muscle sample may be removed either surgically, through a slit made in the skin, or by needle biopsy, in which a thin hollow needle is inserted through the skin and into the muscle. A nerve may be removed through a small surgical incision near the ankle, or occasionally near the wrist.
A brain biopsy, which can help determine the type of tumor a person has and identify certain infections, requires surgery to remove a small piece of the brain or tumor. It is an invasive procedure that carries some risks.
Cerebrospinal fluid analysis
Cerebrospinal fluid analysis involves the removal of a small amount of the fluid that surrounds the brain and spinal cord. The procedure commonly requires a lumbar puncture or spinal tap, which may be done as an inpatient or outpatient procedure. The fluid is tested to detect evidence of brain hemorrhage (bleeding), infection, multiple sclerosis, metabolic diseases, or other neurological conditions.
During a cerebrospinal fluid analysis:
- The person will either lie on one side with their knees pulled up to their chest or lean forward while sitting on a table, bed, or chair.
- The person’s back is cleaned and injected with a local anesthetic.
- The injection may cause a slight stinging sensation.
- Once the anesthetic has taken effect, a special needle is inserted between the vertebrae into the spinal cord and a small amount of fluid (usually about three teaspoons) is withdrawn for testing.
- Most people will only feel a sensation of pressure as the needle is inserted.
- Generally, people are asked to lie flat for 1-2 hours after the procedure to reduce the likelihood that they will get a headache, which can happen after a lumbar puncture due to low spinal fluid levels.
There is a small risk of nerve root injury or infection from a lumbar puncture. The procedure takes about 45 minutes.
Electroencephalography
Electroencephalography, or EEG, monitors the brain’s electrical activity through the skull. EEG helps diagnose seizure disorders and other disorders that affect the brain’s activity. EEGs also evaluate sleep disorders and monitor brain activity when a person has been fully anesthetized or loses consciousness. EEG is a painless, low-risk test that can be done in a doctor’s office or at a hospital or testing facility.
During an EEG:
- The person being tested usually reclines in a chair or on a bed.
- A series of small cup-like electrodes are attached to the scalp with a special conducting paste. The electrodes are attached to wires that carry the electrical signals of the brain to a machine.
- During an EEG, a variety of external stimuli, including bright or flashing lights or certain drugs may be given.
- People may be asked to open and close their eyes, or to change their breathing patterns.
- Changes in brain wave patterns are transmitted from the electrodes to an EEG machine or computer.
- An EEG test usually takes about an hour (including set-up time).
Testing for certain disorders, such as seizure or sleep disorders, may require doing a much longer EEG during sleep, which takes about 4 hours.
In people undergoing evaluation for epilepsy surgery:
- Electrodes may be inserted through a surgical opening in the skull to reduce signal interference. This is called an intracranial electrocorticography (ECoG).
- People stay in a hospital epilepsy monitoring unit while implanted electrodes are in place.
- During this time, the brain is monitored for seizures to figure out where they originate.
- People may also be asked to do certain types of tasks (e.g., reading, speaking, or certain movements) so the ECoG can help identify brain regions that are important for normal function and that should be avoided during the surgery.
Electromyography
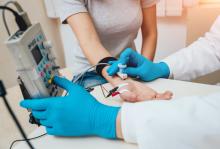
Electromyography, or EMG, can diagnose nerve and muscle disorders, spinal nerve root compression, and motor neuron disorders such as amyotrophic lateral sclerosis (ALS). EMG records the electrical activity in the muscles. Testing may take place in a doctor’s office or clinic.
During an EMG:
- Very fine needles or wires are inserted into a muscle to analyze changes in electrical signals at rest and during movement, which can point to nerve or muscle damage.
- The needles are attached to an EMG machine.
- Testing usually lasts an hour or longer, depending on the number of muscles and nerves to be tested.
- Because of a slight risk of bruising or bleeding, people will be asked if they are on aspirin or blood thinners before they are given EMG.
- Most people find this test to be somewhat uncomfortable.
Nerve conduction study
An EMG is usually done in conjunction with a nerve conduction study (NCS). An NCS measures the nerve’s ability to send a signal, as well as the speed (nerve conduction velocity) and size of the nerve signal.
During an NCS:
- A set of electrodes is taped to the skin over the muscles.
- Wires connect the electrodes to an EMG machine.
- A small electrical pulse (like the sensation of static electricity) is given on the skin a short distance away to stimulate the nerve.
- The electrical signal is viewed on the EMG machine as it travels along the nerve.
- The physician then reviews the nerves’ response to verify any nerve damage or muscle disease.
- There is minimal discomfort and no risk associated with this test.
Electronystagmography
Electronystagmography (ENG) describes a group of tests to diagnose involuntary eye movement, dizziness, and balance disorders. The test is done at a clinic or imaging center.
During an ENG:
- Small electrodes are taped on the skin around the eyes to record eye movements.
- If infrared photography is used instead of electrodes, the person being tested wears special goggles that help record the information.
- Both versions of the test are painless and carry little or no risk.
Evoked potentials
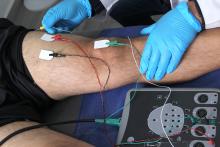
Evoked potentials, also called evoked responses, include three tests that measure the electrical signals to the brain generated by sound, touch, or sight. Evoked potentials test sight and hearing (especially in infants and young children) and can help diagnose multiple sclerosis, spinal cord injury, and acoustic neuroma (small tumors of the acoustic nerve). Evoked potentials also monitor brain activity in coma patients and confirm brain death. Testing may take place in a doctor’s office or hospital setting.
During the procedure:
- One set of electrodes is attached to the person’s scalp with conducting paste. Electrodes may also be attached to other parts of the body, such as the ears, arms, or legs.
- The electrodes measure the brain’s electrical response to auditory, visual, and electrical stimuli.
- A machine records how much time it takes for impulses generated by stimuli to reach the brain.
- Auditory evoked potentials (also called brain stem auditory evoked response) can assess hearing loss and damage to the acoustic nerve and auditory pathways in the brain stem. They can also detect acoustic neuromas. The person being tested sits in a soundproof room and wears headphones. Clicking sounds are delivered one at a time to one ear while a masking sound is sent to the other ear. Each ear is usually tested twice, and the entire procedure takes about 45 minutes.
- Visual evoked potentials detect loss of vision from optic nerve damage (for example from multiple sclerosis). The person sits close to a screen and is asked to focus on the center of a shifting checkerboard pattern. One eye is tested at a time. Each eye is usually tested twice. Testing takes 30-45 minutes.
- Somatosensory evoked potentials (SSEPs) measure responses from electrical stimuli to the nerves. In addition to electrodes on the scalp, electrodes are pasted to the arms, legs, and back to measure the signal as it travels from the peripheral nerves to the brain. Tiny electrical shocks are delivered by electrodes pasted to the skin over a nerve in an arm or leg. SSEPs may help diagnose multiple sclerosis, spinal cord compression or injury, and certain metabolic or degenerative diseases. SSEP tests usually take longer than an hour.
Myelography
Myelography involves the injection of a contrast dye into the spinal canal to enhance imaging of the spine by CT or X-ray. If you have chronic back pain, a doctor will likely suggest a CT scan or MRI first. But if these don’t explain what is causing the pain, a myelogram can show certain issues that a doctor can't see with a CT scan or MRI. For example, myelograms can identify cysts (fluid filled sacs) in the brain and tears in the brain’s dura mater, which can be a complication of surgery or can follow an injury. Myelography can be done as an outpatient procedure at a hospital or medical center.
During myelography:
- Local anesthesia is injected into a site between two vertebrae in the lower back and a small amount of the cerebrospinal fluid is removed by spinal tap.
- Contrast dye is injected into the spinal column and a CT scan or a series of X-rays is taken.
- People may experience some pain during the spinal tap as well as headache following the procedure.
- There is a slight risk of fluid leakage or allergic reaction to the dye.
- The procedure takes about one hour.
Polysomnogram
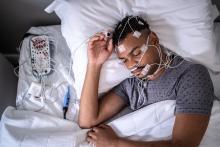
A polysomnogram, also known as a sleep study, measures brain and body activity during sleep. Sleep studies can help diagnose sleep disorders, including restless legs syndrome, periodic limb movement disorder, and insomnia, as well as breathing disorders such as sleep apnea. Polysomnograms are done over one or more nights at a sleep center.
During a polysomnogram:
- Electrodes are attached to the person’s scalp, eyelids, leg, and/or chin.
- Throughout the night and during the various wake/sleep cycles, the electrodes record brain waves, eye movement, breathing, leg and skeletal muscle activity, blood pressure, and heart rate.
- The person may be video recorded to note any movement during sleep.
- Polysomnograms are noninvasive and painless. The most common side effect is skin irritation caused by the adhesive used to attach sensors.
Ultrasound imaging
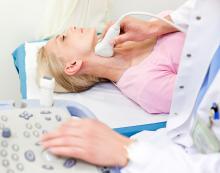
Ultrasound, also called ultrasonography, uses high-frequency sound waves to create images that show inside the body. It can assess changes in the anatomy of soft tissues, including muscle and nerve tissues. It is more effective than an X-ray in showing soft tissue changes, such as tears in ligaments or soft tissue masses. Ultrasounds can be done in a clinic or doctor’s office.
During an ultrasound:
- The person lies on a table or reclines in an examination chair.
- A jelly-like lubricant is applied to the bare skin and a transducer, which sends and receives high-frequency sound waves, is passed over the body.
- The sound wave echoes are recorded and displayed as a real-time visual image of the structure or tissue being examined.
- Ultrasound is painless, noninvasive, and carries little or no risk.
- The test takes 15-30 minutes to complete.
There are many types of ultrasounds relevant to neurological disorders. These include:
- Carotid Doppler ultrasound, which measures blood flow in arteries and blood vessels in the neck.
- Transcranial Doppler ultrasound, which shows blood flow in certain arteries and blood vessels inside the skull. Carotid dopplers and transcranial dopplers can help assess a person’s risk of stroke.
- Duplex ultrasound, which uses two types of ultrasound to see and hear the blood flow in the major arteries and veins in the arms and legs.
X-rays
X-rays of a person’s chest and skull may be taken as part of a neurological evaluation. X-rays can show any part of the body, such as a joint or major organ system. Tissue masses such as injured ligaments or a bulging disc are not visible on conventional X-rays. X-rays can be done in a doctor’s office or clinic and are fast and noninvasive.
In a conventional X-ray:
- A concentrated burst of low-dose ionized radiation passes through the body and onto a photographic plate.
- Since calcium in bones absorbs X-rays more easily than soft tissue or muscle, the bony structure appears white on the film.
- Vertebral misalignment or fractures can be seen within minutes.
Fluoroscopy is a type of X-ray that uses a continuous or pulsed beam of low-dose radiation to produce continuous images of a body part in motion. The fluoroscope (X-ray tube) is focused on the area of interest and pictures are either recorded or sent to a monitor for viewing. Fluoroscopy evaluates swallowing and can be part of other procedures, such as a lumbar puncture, angiogram for clot removal, or myelogram.
What are the latest updates on neurological tests and procedures?
The National Institute of Neurological Disorders and Stroke (NINDS), part of the National Institutes of Health (NIH), is the nation’s leading federal funder of research on neurological disorders. Scientists funded by NINDS seek to develop additional and improved screening methods to confirm a specific diagnosis more accurately and quickly and investigate other factors that might contribute to disease. Technological advances in imaging will allow researchers to better see inside the body and carry less risk to the person getting the procedure. These diagnostics and procedures will continue to be important clinical research tools for confirming a neurological disorder, understanding how disease progresses, and monitoring the effects of treatment.
Where can I find more information about neurological tests and procedures?
For information on neurological disorders or research programs funded by the NINDS, contact us at:
National Institute of Neurological Disorders and Stroke
800-352-9424
The following resources may provide information about neurological diagnostics: